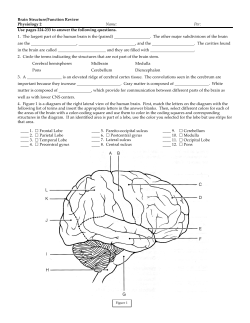
Middle Cerebral Artery Occlusion Compromising the Sensory and Motor Cortices CASE REPORT
K. H. Lin, W. C. Shyu CASE REPORT Middle Cerebral Artery Occlusion Compromising the Sensory and Motor Cortices 1,2 1 Kuan-Hung Lin , Woei-Cherng Shyu 1 2 Department of Neurology , Buddhist Tzu Chi General Hospital, Hualien, Taiwan; Department of Neurology , Chung Gung Memorial Hospital, Taoyuan, Taiwan ABSTRACT We report a patient with mild motor and sensory dysfunction of the face and hand, which was caused by a middle cerebral artery occlusion with infarction in the sensory and motor cortices of the dominant hemisphere. She showed striking recovery in three days. We discuss some of the possible circulatory variants that might underlie this pattern of infarction. (Tzu Chi Med J 2006; 18:382384) Key words: MCA occlusion, infarction, central sulcus, collateral circulation INTRODUCTION Infarctions in the middle cerebral artery (MCA) area may present with different clinical features depending on which divisions or branches are occluded and on the extent of the infarct [1]. If the anterior (superior) division is involved, the most common consequences are contralateral hemiparesis and hemisensory loss. In addition, aphasia usually accompanies lesions in the left hemisphere, whereas sensory neglect phenomena and anosognosia accompany right hemispheric lesions. Here we provide a clinical description of one case of complete left MCA occlusion at the distal part of M1 segment of the dominant hemisphere that only affected the precentral and postcentral gyrui. CASE REPORT An 88 year old right-handed woman without a his- tory of hypertension and previous stroke suffered an acute episode of dizziness and collapse at home when she got up in the early morning. In the emergency room she had mildly slurred speech without aphasia, a shallow right nasolabian fold without dysphagia, numbness over right lower face, right distal hand and moderate weakness of the right arm, but no weakness of the right leg (NIHSS=7). A head CT scan showed only brain diffused atrophy correlated to her old age and a brain MRI scan according to the Diffusion Weighted Image revealed multiple small lacunar infarcts as well as a new left MCA infarct that only involved the precentral and postcentral gyrui. A brain MRA scan showed patent anterior cerebral arteries (ACA), and an attenuated flow-related signal for the left MCA at the distal part of M1 segment; the superior division of this artery was not visualizable. A neck MRA scan and carotid ultrasound were unremarkable. Her neurological deficits improved strikingly and she asked to be discharge after three days hospitalization. Received: March 7, 2006, Revised: April 25, 2006, Accepted: June 7, 2006 Address reprint requests and correspondence to: Dr. Kuan-Hung Lin, Department of Neurology, Buddhist Tzu Chi General Hospital, 707, Section 3, Chung Yang Road, Hualien, Taiwan PUO Tzu Chi Med J 2006 18 No. 5 MCA infarct involving only sensory and motor cortices Fig. 1. (A) Brain MRA showing an occlusion of the left MCA distal M1 branch; the superior division of the left MCA is not visualizable. (B) Brain MRI-DWI revealing an acute infarct in the left lateral precentral gyrus. (C,D,E) Brain MRI-T2, FLAIR, ADC mapping images showed a ischemic lesion in the left lateral precentral gyrus. DISCUSSION The middle cerebral artery is the largest branch of the internal carotid artery. The artery supplies a portion of the frontal lobe and the lateral surface of the temporal and parietal lobes, including the primary motor and sensory areas of the face, throat, hand and arm and in the dominant hemisphere, the areas for speech. The clinical abrupt sensory-motor symptoms over right face and right upper limb of the patient show a possible anatomic Tzu Chi Med J 2006 18 No. 5 PUP K. H. Lin, W. C. Shyu localization of the vascular lesion to the lateral part of the left precentral and postcentral gryus [2,3]. The lateral precentral gyrus contains the motor representation for the contralateral face and arm and the lateral postcentral gyrus contains the sensory functions. Both of them are normally supplied by a distal branch of the middle cerebral artery, the lateral Rolandic artery [4]. This area is normally included in all infarctions involving the superior division of the MCA. In order to explain the sparing of other branch of the MCA observed in this case of MCA occlusion, at least four different mechanisms may be suspected. In the first, a shower of small emboli resulting from the break up of a large proximal embolus would block distal branches of the MCA. Only precentral and postcentral gryus underwent ischemic infarction and the other areas of the cortices were spared because of spontaneous emboli lysis except for the lateral Rolandic artery. However, in previously reported embolic cases of this type, the hemiparesis was dense initially and improved subsequently, namely a "spectacular shrinking deficit" [5,6]. However, in this case, the motor deficit was minimal at presentation, which therefore does not support this model for the mechanism. A second possibility is spontaneous local recanalization of the occluded vessels, with or without additional good leptomeningeal collateralization, which could lead to selective restoration of flow except for the lateral Rolandic branch of the MCA. This would be able to explain the rapid recovery after the initial focal weakness and numbness. Recanalization occurring within the first few days after an acute event is known to improve the outcome after MCA infarction. However, further MRA follow-up would be required after the initial stroke to show that recanalization has occurred. A third possibility is the presence of pre-existing collateral circulation established because of chronic poor MCA perfusion [7-9], except for the lateral Rolandic branch. This would provide a reasonable explanation for isolated Rolandic infarct effect of the MCA occlusion in this patient. Unfortunately, we were unable to demonstrate such selective collateral circulation, because our patient did not receive conventional angiography due to her age. Without this information, other potential changes including the possibility of an embolus break up with distal migration, as described in situation 1 above, cannot be entirely ruled out. The final possible explanation for pathogenesis of the cortical infarction resulting from MCA occlusion is that it is the result of a combination of multiple stroke mechanisms, such as both local branch occlusion and embolism [10,11]. To confirm this hypothesis, there PUQ would be a need for serial DWI/MRA imaging and microembolic signal monitoring by transcranial Doppler in order to provide supportive evidence. In conclusion, we suggest that further prospective studies of similar patients using catheter angiography or follow-up MRA are necessary because they might reveal how such a stroke mechanism might be exploited to improve the treatment. REFERENCES 1. Ringelstein EB, Biniek R, Weiller C, Ammeling B, Nolte PN, Thron A: Type and extent of hemispheric brain infarctions and clinical outcome in early and delayed middle cerebral artery recanalization. Neurology 1992; 42:289-298. 2. Seitz RJ, Hoflich P, Binkofski F, Tellmann L, Herzog H, Freund HJ: Role of the premotor cortex in recovery from middle cerebral artery infarction. Arch Neurol 1998; 55: 1081-1088. 3. Portera-Cailliau C, Doherty CP, Buonanno FS, Feske SK: Middle cerebral artery territory infarction sparing the precentral gyrus: Report of three cases. J Neurol Neurosurg Psychiatry 2003; 74:510-512. 4. Racy A, Jannotta FS, Lehner LH: Aphasia resulting from occlusion of the left anterior cerebral artery. Report of a case with an old infarct in the left Rolandic region. Arch Neurol 1979; 36:221-224. 5. Minematsu K, Yamaguchi T, Omae T: 'Spectacular shrinking deficit': Rapid recovery from a major hemispheric syndrome by migration of an embolus. Neurology 1992; 42:157-162. 6. Kraemer N, Thomalla G, Soennichsen J, et al: Magnetic resonance imaging and clinical patterns of patients with 'spectacular shrinking deficit' after acute middle cerebral artery stroke. Cerebrovasc Dis 2005; 20:285290. 7. Wei L, Erinjeri JP, Rovainen CM, Woolsey TA: Collateral growth and angiogenesis around cortical stroke. Stroke 2001; 32:2179-2184. 8. Mull M, Schwarz M, Thron A: Cerebral hemispheric lowflow infarcts in arterial occlusive disease. Lesion patterns and angiomorphological conditions. Stroke 1997; 28:118-123. 9. Coyle P: Spatial relations of dorsal anastomoses and lesion border after middle cerebral artery occlusion. Stroke 1987; 18:1133-1140. 10. Caplan LR, Hennerici M: Impaired clearance of emboli (washout) is an important link between hypoperfusion, embolism, and ischemic stroke. Arch Neurol 1998; 55: 1475-1482. 11. Lee DK, Kim JS, Kwon SU, Yoo SH, Kang DW: Lesion patterns and stroke mechanism in atherosclerotic middle cerebral artery disease: Early diffusion-weighted imaging study. Stroke 2005; 36:2583-2588. Tzu Chi Med J 2006 18 No. 5
© Copyright 2026